Deep Brain Stimulation for Parkinson’s Disease
What is Deep Brain Stimulation for Parkinson’s Disease?
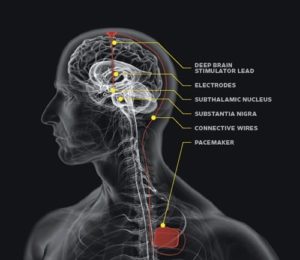 Deep brain stimulation (DBS) is a surgical procedure used to treat a variety of disabling neurological symptoms—most commonly the debilitating symptoms of Parkinson’s disease (PD), such as tremor, rigidity, stiffness, slowed movement, and walking problems. The procedure is also used to treat essential tremor, a common neurological movement disorder. At present, the procedure is used only for patients whose symptoms cannot be adequately controlled with medications.
Deep brain stimulation (DBS) is a surgical procedure used to treat a variety of disabling neurological symptoms—most commonly the debilitating symptoms of Parkinson’s disease (PD), such as tremor, rigidity, stiffness, slowed movement, and walking problems. The procedure is also used to treat essential tremor, a common neurological movement disorder. At present, the procedure is used only for patients whose symptoms cannot be adequately controlled with medications.
DBS uses a surgically implanted, battery-operated medical device called a neurostimulator—similar to a heart pacemaker and approximately the size of a stopwatch—to deliver electrical stimulation to targeted areas in the brain that control movement, blocking the abnormal nerve signals that cause tremor and PD symptoms.
Before the procedure, a neurosurgeon uses magnetic resonance imaging (MRI) or computed tomography (CT) scanning to identify and locate the exact target within the brain where electrical nerve signals generate the PD symptoms.
 Some surgeons may use microelectrode recording—which involves a small wire that monitors the activity of nerve cells in the target area—to more specifically identify the precise brain target that will be stimulated. Generally, these targets are the thalamus, subthalamic nucleus, and globus pallidus.The DBS system consists of three components: the lead, the extension, and the neurostimulator.
Some surgeons may use microelectrode recording—which involves a small wire that monitors the activity of nerve cells in the target area—to more specifically identify the precise brain target that will be stimulated. Generally, these targets are the thalamus, subthalamic nucleus, and globus pallidus.The DBS system consists of three components: the lead, the extension, and the neurostimulator.
The lead (also called an electrode)—a thin, insulated wire—is inserted through a small opening in the skull and implanted in the brain. The tip of the electrode is positioned within the targeted brain area.

The extension is an insulated wire that is passed under the skin of the head, neck, and shoulder, connectng the lead to the neurostimulator.
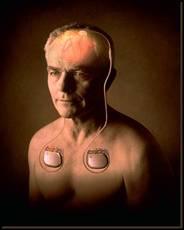
 The neurostimulator (the “battery pack”) is the third component and is usually implanted under the skin near the collarbone. In some cases it may be implanted lower in the chest or under the skin over the abdomen.
The neurostimulator (the “battery pack”) is the third component and is usually implanted under the skin near the collarbone. In some cases it may be implanted lower in the chest or under the skin over the abdomen.
Once the system is in place, electrical impulses are sent from the neurostimulator up along the extension wire and the lead and into the brain. These impulses interfere with and block the electrical signals that cause PD symptoms.
 Unlike previous surgeries for PD, DBS does not damage healthy brain tissue by destroying nerve cells. Instead the procedure blocks electrical signals from targeted areas in the brain. Thus, if newer, more promising treatments develop in the future, the DBS procedure can be reversed. Also, stimulation from the neurostimulator is easily adjustable—without further surgery—if the patient’s condition changes. Some people describe the stimulator adjustments as “programming.”
Unlike previous surgeries for PD, DBS does not damage healthy brain tissue by destroying nerve cells. Instead the procedure blocks electrical signals from targeted areas in the brain. Thus, if newer, more promising treatments develop in the future, the DBS procedure can be reversed. Also, stimulation from the neurostimulator is easily adjustable—without further surgery—if the patient’s condition changes. Some people describe the stimulator adjustments as “programming.”
What is the prognosis?
Although most patients still need to take medication after undergoing DBS, many patients experience considerable reduction of their PD symptoms and are able to greatly reduce their medications. The amount of reduction varies from patient to patient but can be considerably reduced in most patients. The reduction in dose of medication leads to a significant improvement in side effects such as dyskinesias (involuntary movements caused by long-term use of levodopa). In some cases, the stimulation itself can suppress dyskinesias without a reduction in medication.
